Latest News
A/Prof Sophie Payne discusses vagus nerve stimulation on Triple R’s Einstein A Go-Go
A/Prof Sophie Payne recently joined Dr Shane Huntington on Melbourne radio program Einstein A Go-Go to discuss emerging research into vagus nerve stimulation and how implantable bioelectronic technologies developed at the Bionics Institute could one day help people living with a vast array of conditions.
As Head of the Vagus Nerve Stimulation Centre of Excellence at the Institute, Sophie spoke about the role of the vagus nerve in regulating inflammation and explained how her research team has developed a new approach to stimulation targeting the abdominal vagus nerve.
Understanding the vagus nerve
During the interview, Sophie described the vagus nerve as one of the body’s major communication pathways, connecting the brain to organs including the heart, lungs and digestive system.
“The word vagus actually comes from Latin, which means ‘to wander’,” Sophie explained. “And it does just that through your body.”
“Its main role is to allow you to rest and digest. But we now know it also has a huge role in controlling your body’s natural anti-inflammatory pathways.”
Investigating inflammation and immune regulation
Researchers at the Bionics Institute are particularly interested in how vagus nerve signaling may help regulate inflammation in diseases such as Crohn’s disease and rheumatoid arthritis.
Sophie says the body rapidly detects inflammation and sends signals through the vagus nerve to the brain, triggering natural anti-inflammatory pathways.
“The vagus nerve acts like a brake on the body to moderate and regulate the immune system because it can just go absolutely nuts.”
Developing a new stimulation approach
One of the key topics discussed during the interview was the implantable vagus nerve stimulation device being developed at the Bionics Institute by Sophie’s research team.
Traditional vagus nerve stimulation therapies are commonly delivered at the neck. Sophie explained that the Institute’s approach instead targets the abdominal vagus nerve.
“When you stimulate the vagus nerve [at the abdomen], you don’t get issues with activating your vital organs like your heart and your lungs,” she said.
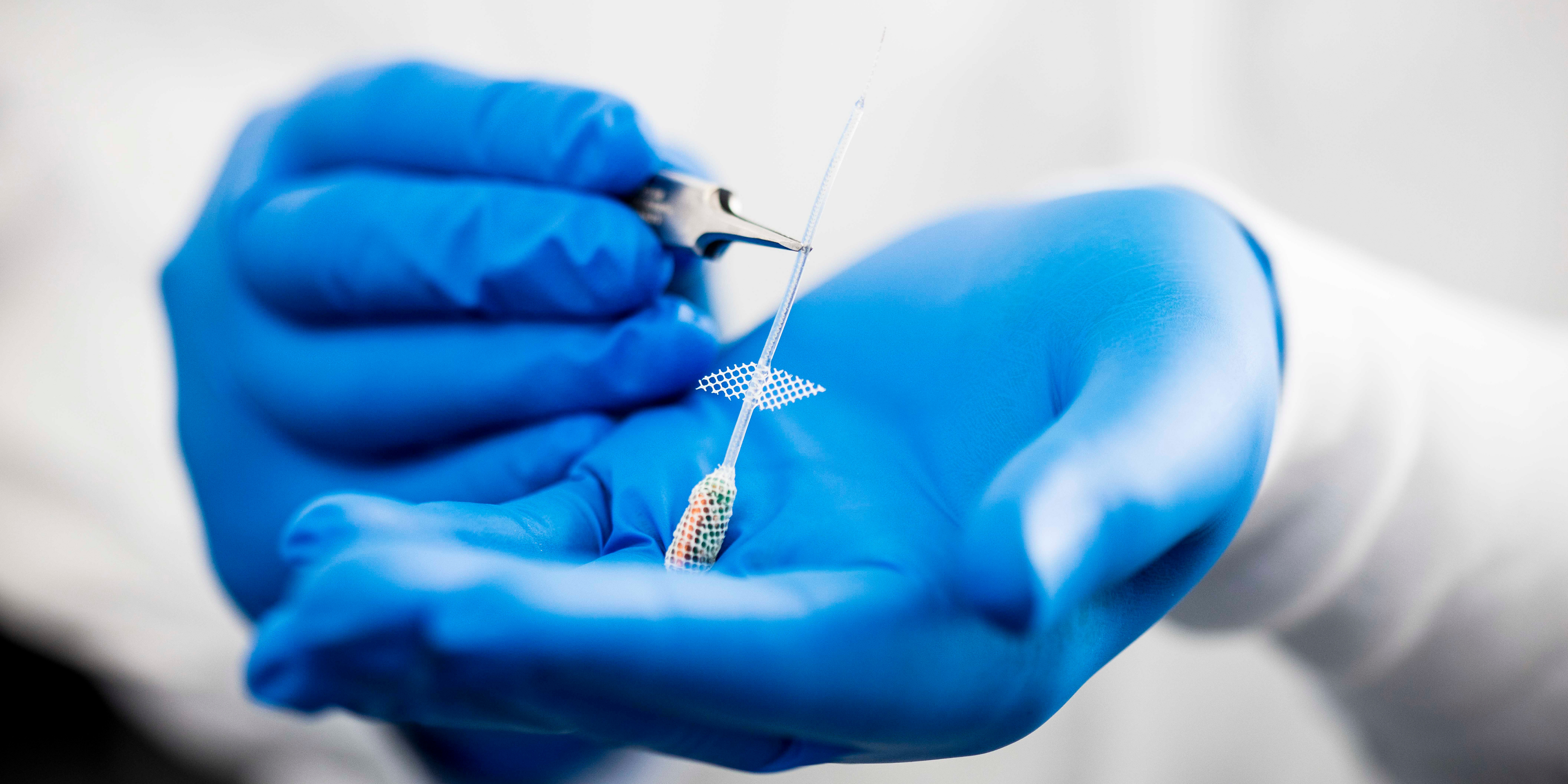
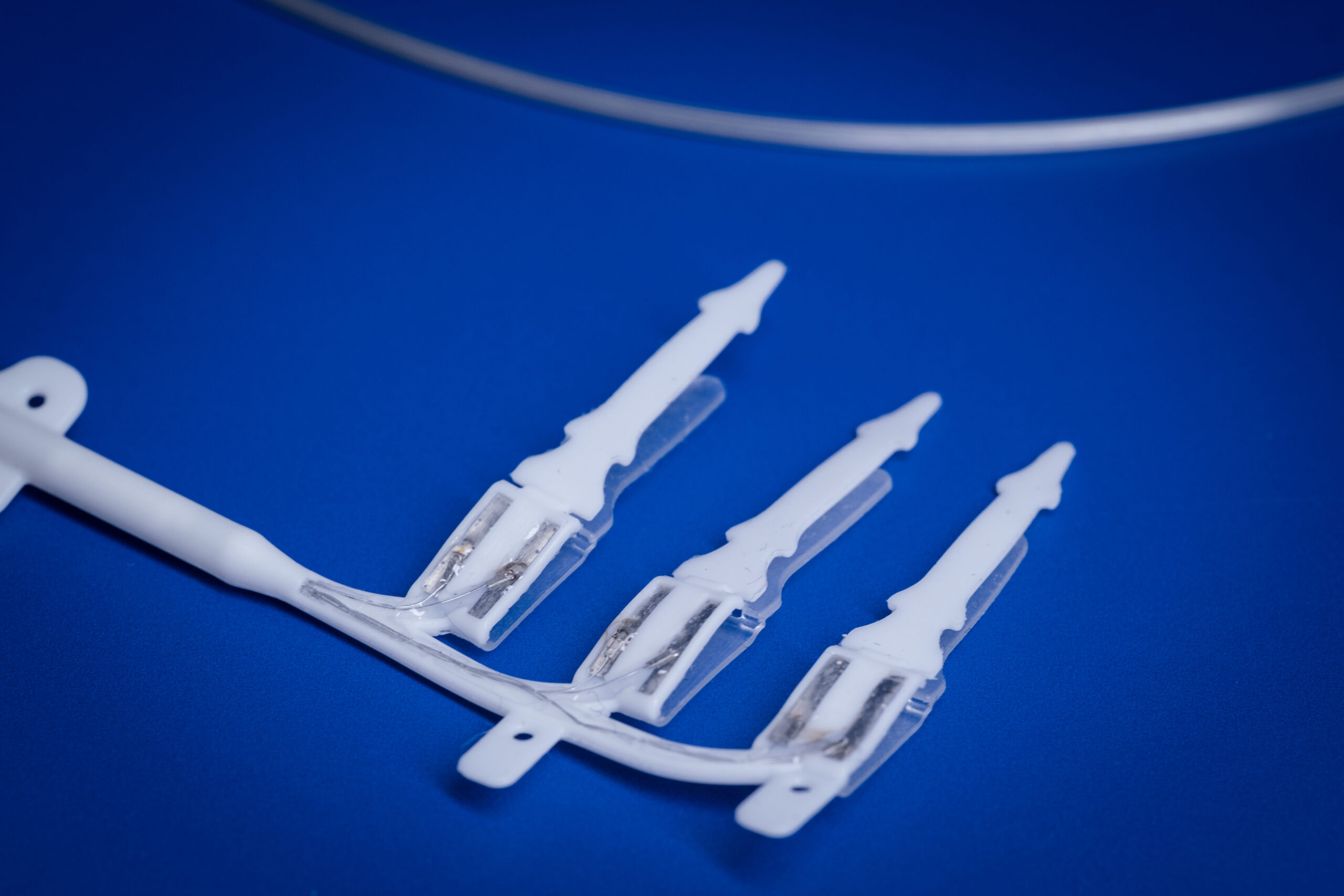
The implant is inserted using keyhole surgery and includes electrodes placed around the abdominal vagus nerve, along with a battery pack implanted near the hip.
“It’s a tiny little device, about the size of your little fingernail,” Sophie said.
Describing the implant, she explained that the electrodes “sort of clamp around the nerve like a bookmark in a book”.
The device delivers electrical stimulation designed to activate the body’s natural anti-inflammatory pathways without the side effects associated with stimulation at neck level.
Looking ahead
Beyond stimulation itself, Sophie said researchers are also exploring ways to record vagus nerve activity in real time.
“We’re also looking at, not just ways to activate the nerve, but also to listen to it,” she said.
“If the body is very inflamed and the vagus nerve is signalling in a certain way… we know we’ve got to stimulate.”
Clinical trials involving vagus nerve stimulation for Crohn’s disease and rheumatoid arthritis are ongoing, while other applications discussed during the interview — including chronic pain caused by endometriosis and migraines — remain in earlier stages of investigation.
We have a research pipeline geared towards trying to get this technology into clinic as quickly as possible if it’s going to be a viable, useful, meaningful therapy Associate Professor Sophie Payne
The Vagus Nerve Stimulation Centre of Excellence was established to explore the full potential of vagus nerve–based treatments. Often described as a window to the brain, the vagus nerve provides a pathway for advancing research into neurological conditions including epilepsy, Parkinson’s disease and stroke, while also supporting the development of new therapies for inflammation-based diseases such as endometriosis.
Listen to the full interview
Hear Associate Professor Sophie Payne in conversation on Einstein A Go-Go via Triple R 102.7FM.
You might be interested in…
Support Us
Invest in groundbreaking research to help those with Parkinson’s disease gait
Donate nowAbigail’s Story
Abigail is a single mother to two young daughters and was diagnosed with Parkinson’s disease at 40.
Each day, she waits for medication to take effect before starting basic routines like the school run, yet walking remains painful and unsteady. Her movement can be uneven and unpredictable, increasing the risk of trips and falls, especially in busy or unfamiliar environments.
Despite these challenges, Abigail remains focused on her children and continues to stay involved in their daily lives. Parkinson’s also affects her energy, memory and ability to manage the demands of parenting, making everyday tasks more difficult.
Parkinson’s gait impairment has a profound impact on Abigail’s quality of life, independence and her capacity to provide for her daughters.
Our research into a new non-invasive treatment could be the solution for Abigail.


Parkinson’s gait research can change lives
For someone with Parkinson’s gait impairments, movement becomes a challenge. Walking becomes painful. The resulting shuffling gait can lead to falls, hospital, even early admission to aged care.
Now there’s promising research to relieve this problem. Here’s how it works:
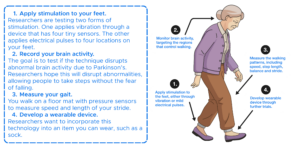
Help fund pioneering research
Parkinson’s disease affects more than six million people worldwide, and gait difficulties are among its most common and debilitating symptoms.
Our research team, led by A/Prof Mehrnaz Shoushtarian, is developing a new intervention to address these challenges using non-invasive stimulation of the feet, delivered through vibration or mild electrical pulses.
The team is currently conducting clinical trials to test whether this approach can reduce gait disturbances by disrupting the abnormal brain activity that interferes with walking.
You can help make this work possible with a generous gift today—supporting efforts to reduce falls and improve stability for people living with Parkinson’s.


Imagine if you could put on a sock and it buzzed your feet and then you could walk more smoothly during the day… that would be amazing. This gives us a lot of hope.” Abigail, whose early onset of Parkinson’s affected her ability to walk independently and care for her children.
Want to support research like this?
Want to support the future of research like this?
The progress of life-changing treatments are only made possible by donations from our supporters. Your support today could give those with chronic pain hope of a pain-free future.
Find out how you can support research innovation here.


Latest News
Philip Binns appointed Chair of the Bionics Institute Board
The Bionics Institute is pleased to announce the appointment of Mr Philip Binns as Chair of the Board.
Phil brings more than 30 years of leadership experience across the scientific and life sciences industries. He most recently served as President of Agilent Technologies’ Life Sciences and Applied Markets Group, retiring in April 2025 after a distinguished global career.
Phil has been a valued member of the Bionics Institute Board and brings deep expertise in technology, commercialisation and innovation. His experience working across the life sciences sector will help guide the Institute as it continues to translate cutting-edge research into medical technologies that transform lives.
Phil will be supported by Deputy Chair, Hannah Crawford whose leadership, financial acumen and strategic expertise have been instrumental in supporting the Institute’s growth and ensuring robust oversight across all areas.
It is an honour and privilege to take on the role of Chair of the Bionics Institute. The Institute has an exciting future, building on the many years of incredible innovations from our world class research team. I look forward to working with the team and our partners to further our mission of developing and bringing to clinic new life-changing diagnostics and therapies for people living with challenging medical conditions.
In addition to his role with the Bionics Institute, Phil is Chair of Epiminder Ltd, a board member of Lightcast Discovery Ltd, and serves as a National Advisory Councillor for the Australian Industry Group. He is also an active investor and mentor supporting early-stage technology companies.
You might be interested in…
Latest News
Meet Dr Hamish MacDougall
I think that all Australians, regardless of where they live, should have access to accurate medical diagnoses and interventions. When it comes to basic access to specialist care in remote and rural locations, the playing field really needs to be levelled.
With an exciting career that includes a stint at NASA, Dr Hamish MacDougall’s professional career has been defined by a string of inventions fuelled by curiosity and a desire to improve neurological conditions. He has now joined the Bionics Institute, where he is working on an extended reality (XR) device solution for the diagnosis of neurological conditions.
We sat down with Hamish for a conversation about his research.
Why did you join the Bionics Institute?
What really drew me to the Bionics Institute is how different it is to other organisations. Because my research is dependent on being able to get devices out into the public, into the lives of people who need them, I wanted to work somewhere that not only understood the value and necessity of commercialisation, but also had the experience and the success to make it happen.
At the start of my career, I thought science just about the endless cycle of creating a gadget and publishing a paper about it, then putting the gadget in a box on a shelf and starting the process all over again. But, seeing the gaps that exist in healthcare makes you realise just how valuable it is to get those devices off the shelves and into the world.
Commercialisation is the only real pathway for doing that, getting a gadget from a bench in the lab into tens of thousands of clinics. I can’t physically make thousands of prototypes; you need a commercial partner for that. The Bionics Institute really understands that pathway, and that’s why I chose to come here.
Tell us a bit about what you’re working on right now.
My main project at the moment uses Extended Reality (XR) – the umbrella term that includes virtual reality, mixed reality and augmented reality. I have developed a XR headset which is capable of administering a huge variety of tests and can be remotely accessed from anywhere.
What this means is, we can send this headset out to, say, a remote clinic in rural NT, and the GP out there can put this headset on a patient who’s having a vision or neurological problem. The GP can then go and make himself a coffee, or do some paperwork for half an hour, while a specialist working out of a hospital here in Melbourne can communicate with the individual and run tests in real time.
The tests will show up on the screen for the patient to follow with their eyes, and the data captured about their eye movements can be sent back to the specialist in real time for analysis.
It means we can move it away from subjective, conversational diagnosis and into real, definitive data that clinicians can use for accurate diagnosis.
How does it differ from what currently exists in clinics?
The first difference is cost, which is obviously a concern. The current options that can do a similar thing are around $100,000. Second is the testing capabilities. These goggles can do many different tests, which has the potential to open up lots of new avenues. Ophthalmologists, for example, don’t currently have anything like this that they can use for testing and analysis. And third is, of course, the portability.
When you put all three differences together, that intersection is where the possibilities really open up. That’s what I find so exciting. Imagine being able to send these out on every plane with the Royal Flying Doctor Service, or the Fred Hollows Foundation. We’re talking about something that fits in a case not much bigger than a lunchbox. A social worker could throw it in the passenger seat of their car when they go out to visit people. The possibilities are endless.
What makes this so important?
I think that all Australians, regardless of where they live, should have access to accurate medical diagnoses and interventions. When it comes to basic access to specialist care in remote and rural locations, the playing field really needs to be levelled.
I read an article in the ABC last year that was talking about people in every state waiting years to see a neurologist. And that’s against a recommended wait time of no more than 30 days. People are not only suffering through their original symptoms for this time, but on top of that we’re finding that they are developing additional complications, often irreversible ones.
I remember reading a similar article a couple of years ago, and things seem to only have gotten worse since then. It’s a problem that is growing and needs new solutions to address it.
What is standing in the way of making this happen? What’s the biggest obstacle you need to solve right now?
All government grants have this kind of roadblock in them, where you need to have a certain amount of data to get this happening in order to get money. But you need money to do the work that gets you the data.
Right now, we need to get our devices in front of vestibular clinicians. They’re the experts; they’re the ones who are in front of patients every day. We need their support in order to take this device further. So, we need the money to manufacture enough devices to send out to these clinicians and then partner with them to do the trials that can give us the data that informs us about how to proceed.
That’s where the support of philanthropy comes in, that’s what gets us across the line and gets us to a point where we have something that says to the government, or a company ‘hey, this is actually possible, this can happen, and now we can pass the baton to you and you can put it out into the world, bring it to the public.’
That’s what we ask for when we ask for people to help us: bridge the gap between what we have now, and what government funding gives us.
You might be interested in…
Latest News
Bionics Institute CEO honoured at Impact Investment Summit 2026
The Bionics Institute is proud to celebrate CEO Robert Klupacs, who has been recognised with an Individual Outstanding Achievement Award at the 2026 Impact Investment Awards.
This national recognition highlights Robert’s and Bionics Institute’s leadership in advancing medical technology research and our innovative approach to funding life-changing discoveries.
By bringing together philanthropy, impact investment and intellectual property licensing, Robert and Bionics Institute has helped accelerate the development of technologies that have the potential to improve lives on a global scale.
The awards were of the Impact Investment Summit held in Sydney on March 25/26.
\With over 850 attendees, the event connected investors with high-impact opportunities across sectors including healthcare, medtech and social innovation.
The Summit plays a key role in mobilising capital toward solutions that deliver measurable benefits for communities and patients, aligning closely with the Bionics Institute’s mission to translate research into real-world outcomes.
Under Robert’s leadership, the Institute continues to push the boundaries of what’s possible in hearing and neurological research—ensuring that breakthrough science can reach the people who need it most, faster.
Robert was recognised alongside an inspiring group of leaders, including Georgina Byron AM, CEO of the Snow Foundation; Hanna Ebeling CFA, CEO at SEFA; and Sally McCutchan OAM.
We also extend our congratulations to all organisations recognised at this year’s awards.
This recognition reflects not only individual achievement, but the growing importance of innovative funding models in bringing medical research to life—turning promising ideas into tangible health outcomes.
To learn more about the awards and the Impact Investment Summit, visit: https://impactinvestmentsummit.com/
You might be interested in…
Latest News
One step closer to personalised cochlear implant care
Researchers at the Bionics Institute are advancing a new frontier in hearing healthcare, with significant progress in the development of digital twin technology for cochlear implant users.
The team has successfully developed and validated a sophisticated virtual model of the electrode–neuron interface—an essential component in understanding how cochlear implants stimulate the auditory nerve.
This provides a reliable foundation for simulating how individual patients respond to implant settings, moving beyond traditional, moving beyond traditional, one-size-fits-all approaches to programming.
Building on this work, researchers are now integrating machine learning techniques to predict personalised programming parameters.
These AI-driven models are designed to account for the unique anatomy and neural responses of each user, enabling more precise, adaptive, and data-driven management of cochlear implants.
The ultimate goal is to create fully realised “twins” of cochlear implant patients: virtual replicas that can be used to test and optimise device settings before applying them in clinical practice.
This approach has the potential to significantly improve outcomes, particularly for patients who may struggle to provide consistent feedback during standard programming sessions, such as young children.
Clinical validation of these digital twin models is expected to begin in the coming year, representing a critical step toward their integration into real-world healthcare settings.
If successful, the technology could streamline clinical workflows, reduce the need for repeated adjustments, and deliver more consistent and effective hearing outcomes.
As artificial intelligence continues to reshape medicine, this work highlights how digital twin technology can move personalised care from concept to practice, offering a smarter, more tailored approach to cochlear implant management.
To find out more about this research click here.
You might be interested in…
Latest News
From cruise ship lectures to championing brain research
“Talking is the simplest yet the most effective means to make a difference,” says Omnia, who travels the world giving lectures that explore the fascinating workings of the human mind.
Onboard cruise ships, she captivates audiences with stories about psychopathy, neuroscience, and the brain—sparking curiosity in people from all walks of life.
It all began after she retired from running her consulting business in psychological and marketing profiling. While on a cruise, she noticed that guests could not stop discussing a criminal case in Victoria.
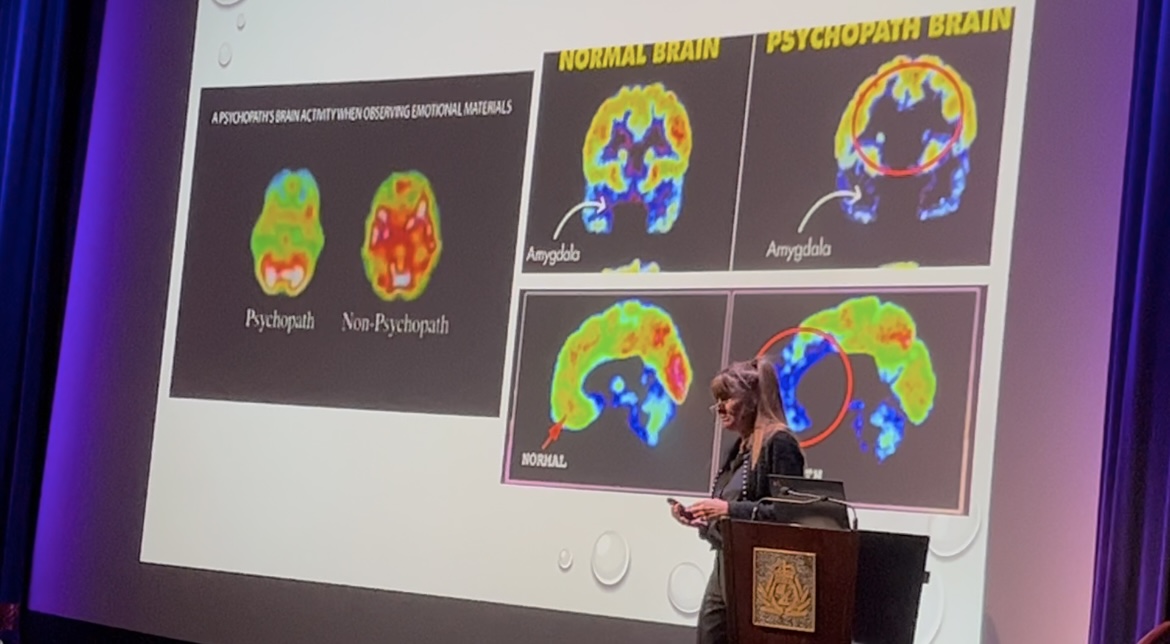
Seeing the international fascination, she developed a series of lectures on the “Mind of a Psychopath,” combining storytelling with brain science.
She shows PET scans of psychopaths, highlighting two brain areas where neurons aren’t firing, linked to guilt, remorse, empathy, and fear.
“After discussing the PET scans, I introduce the Bionics Institute and the work they are undertaking,” she explains.
She shares the Institute’s pioneering research in brain stimulation and clinical trials aimed at conditions such as Alzheimer’s disease, sparking interest without the overwhelm of technical detail.
Audiences respond with fascination.
Her talks create an opportunity to connect a global audience with the important work being done right in her home city: “I am proud that the Bionics institute is in my local Melbourne.”
For Omnia, supporting the Institute is deeply personal. With decades of experience in rigorous research and clinical trials, and a daughter working at the Bionics Institute, she understands both the scientific and human impact of the work being done.
She explains, “People from all walks of life are fascinated with the brain,” adding that Alzheimer’s disease is something we more than likely have been or will be affected by.
Ultimately, Omnia believes in the power of conversation.
When we talk, we become an advocate with the cause, a believer of the cause and a credible spokesperson for the cause.
Through her lectures, she demonstrates that raising awareness doesn’t always require a stage or a campaign and sometimes, it starts with a conversation. Conversations that Omnia proves, can inspire interest, engagement, and support for groundbreaking brain research.
You might be interested in…
Latest News
From graduate to benefactor: A shared mission to make the world better
Anita Castan and Bionics Institute researcher Dr Oscar Murphy both went to the same university 34 years apart. Their degrees took them on different journeys, but they share a common goal: the determination to make the world a better place.
Anita set up a philanthropic foundation in 2022, and says she supports upcoming scientists because she believes in the power of research to make a meaningful difference in the community.
Oscar’s PhD focused on investigating how brain stimulation can be used to treat depression.
He then joined the Bionics Institute in 2022 working in the team led by Professor Kate Hoy, which is running a world-first clinical trial of personalised Transcranial Magnetic Stimulation (TMS) as a potential non-invasive treatment for Alzheimer’s disease.
When Anita met Oscar in 2025, she could see how passionate he was about his work and she was fascinated by the technology.
I have seen first-hand how devastating Alzheimer’s is, not just for the person with the condition but also for their loved ones, and I was keen to support Oscar in his research. It seems that the current treatments don’t work and if TMS could give people with Alzheimer’s their memory back, that would be wonderful. Anita Castan
Oscar was ‘blown away’ when Anita said she wanted to support his research.
He said: “I have spent countless hours writing grant applications that have less than 1 in 10 chance of success and it’s very disheartening to get constant knock backs. I just want to do research to improve quality of life for people and Anita’s gift allows me to do just that. I’m incredibly proud to hold the title of: Anita Castan Foundation Fellow.“
Bionics Institute CEO Robert Klupacs says the link between Anita and Oscar is very special. “Anita wants to make the world a better place and Oscar is working everyday to make the world a better place for people Alzheimer’s – we’re thrilled to partner with Anita to make this a reality.”
You might be interested in…
Latest News
Vagus nerve stimulation research boosted with NHMRC funding
Research at the Bionics Institute Vagus Nerve Stimulation Centre of Excellence (VNSCoE) will be boosted by government grants totalling almost $2.2 million recently awarded by the National Health and Medical Research Council (NHMRC).
Bionics Institute Chief Technology Officer, Professor James Fallon will lead a NHMRC Development Grant project in collaboration with the industry partner that manufactures the implantable pulse generator of the Bionics Institute’s vagus nerve stimulation device, with the aim of accelerating translation of the device into the clinic.
Head of the VNS CoE, A/Prof Sophie Payne will lead an Ideas Grant project with Dr Tomoko Hyakumura, A/Prof Peta Grigsby and Dr Alex Thompson with the aim of understanding how vagus nerve stimulation at abdominal level activates the brain to abate seizures in epilepsy.
In a funding landscape where only 8% of NHMRC grants were successful in 2025, we are delighted to receive significant funding for this vital research, which could change the lives of millions of people around the world with challenging conditions. Robert Klupacs, Bionics Institute CEO
The Centre of Excellence brings together specialised teams of engineers, scientists and clinicians with international and Australian collaborators to investigate the viability of the VNS device as a treatment for over 20 conditions.
The device is currently in clinical trials for Crohn’s disease and rheumatoid arthritis, and under investigation for the treatment of epilepsy and Parkinson’s disease with more in the pipeline.
For more information about the VNSCoE, go to: https://www.bionicsinstitute.org/our-research/vagus-nerve-stimulation-research/
You might be interested in…
Latest News
Announcing new Bionics Institute Board Directors
Celebrating 40 years since the Bionics Institute was founded, we are delighted to announce that three new Directors from Swinburne University of Technology recently joined the Bionics Institute Board.
Interim Chair of the Board Hannah Crawford says the new Directors will bring expertise in research strategy, commercialisation and transdisciplinary research to the Board, helping to propel the Bionics Institute into the future.
This marks the beginning of our partnership with Swinburne where we will combine cutting edge facilities, scientific expertise and resources to progress medical device innovation with the aim of improving human health. Hannah Crawford, Interim Chair
Professor Karen Hapgood is Deputy Vice Chancellor for Research at Swinburne, where she leads Swinburne’s Research strategy and advances Swinburne’s innovative and tech-focused R&D community. Her career has combined industry experience in the USA and Australia, including 4 years of pharmaceutical R&D and manufacturing experience with Merck & Co USA followed by 15 years of leadership roles in the higher education sector, all based around a common thread of manufacturing and STEM and leadership.
Dr Werner van der Merwe is the inaugural Vice President, Innovation and Enterprise at Swinburne, charged with invigorating innovative spirit in partnership with industry. Since his appointment, Swinburne has become one the most inventive universities in Australia and owns shares in more startups for its size than any other Australian university. Before joining Swinburne, Werner led the Commercialisation function at CSIRO, as well as an extensive international career in roles that spanned engineering, research and development, and commercial positions.
As Pro Vice Chancellor, Flagship Initiatives at Swinburne, Professor Alan Duffy is tasked with driving large and ambitious transdisciplinary research across Swinburne’s flagship research areas by actively engaging with external organisations (including government, industry, NGOs) to identify large-scale opportunities that require university-wide collaboration and the formation of coalitions of universities and partners. He brings to the Bionics Institute his experience of over 15 years of research, as a computational astrophysicist, and founder of a sensor company, mDetect, exploring mine sites nationwide.
For more information about our strategic alliance, read this article: https://www.bionicsinstitute.org/latest-news-newsletter/swinburne-bionics-institute-strategic-alliance/