Revolutionising prosthetics: Groundbreaking achievement as bionic hand merges with user’s nervous and skeletal systems, remaining functional after years of daily use
The long-term integration of a bionic hand into the user’s nervous and skeletal systems has been reported as successful for the first time in a patient with a below-elbow amputation.
Karin – a Swedish woman who lost her right hand in a farming accident – was implanted with a novel human-machine interface into her residual bone, nerves, and muscles in December 2018.
The residual limb was surgically modified to better integrate with a bionic hand that uses artificial intelligence (AI) to understand her commands.
The research was led by Professor Max Ortiz Catalán, Head of Neural Prosthetic Research at the Bionics Institute in Australia and Founder of the Center for Bionics and Pain Research (CBPR) in Sweden.
The study was published today in the journal Science Robotics and involved researchers in Sweden, Italy, and Australia.
Life-changing impact of bionic technologies
Karin’s life took a dramatic turn when a farming accident claimed her right arm over 20 years ago. An injury which caused excruciating phantom limb pain.
“It felt like I constantly had my hand in a meat grinder, which created a high level of stress and I had to take high doses of various painkillers,” she says.
In addition to her intractable pain, she found that conventional prostheses were uncomfortable and unreliable, and thus of little help in daily life.
All this changed when she received groundbreaking bionic technology that allowed her to wear a much more functional prosthesis comfortably all day.
The higher integration of the prosthetic hand and Karin’s residual limb also relieved her pain and has been life changing.
“I have better control over my prosthesis, but above all, my pain has decreased. Today, I need much less medication,” Karin says.

A Remarkable Fusion of Human and Machine
Mechanical attachment and reliable control of prosthetic limbs are two of the biggest challenges in artificial limb replacement.
People with limb loss often reject even the sophisticated prostheses commercially available because of these reasons, meaning painful and uncomfortable attachment with limited and unreliable controllability.
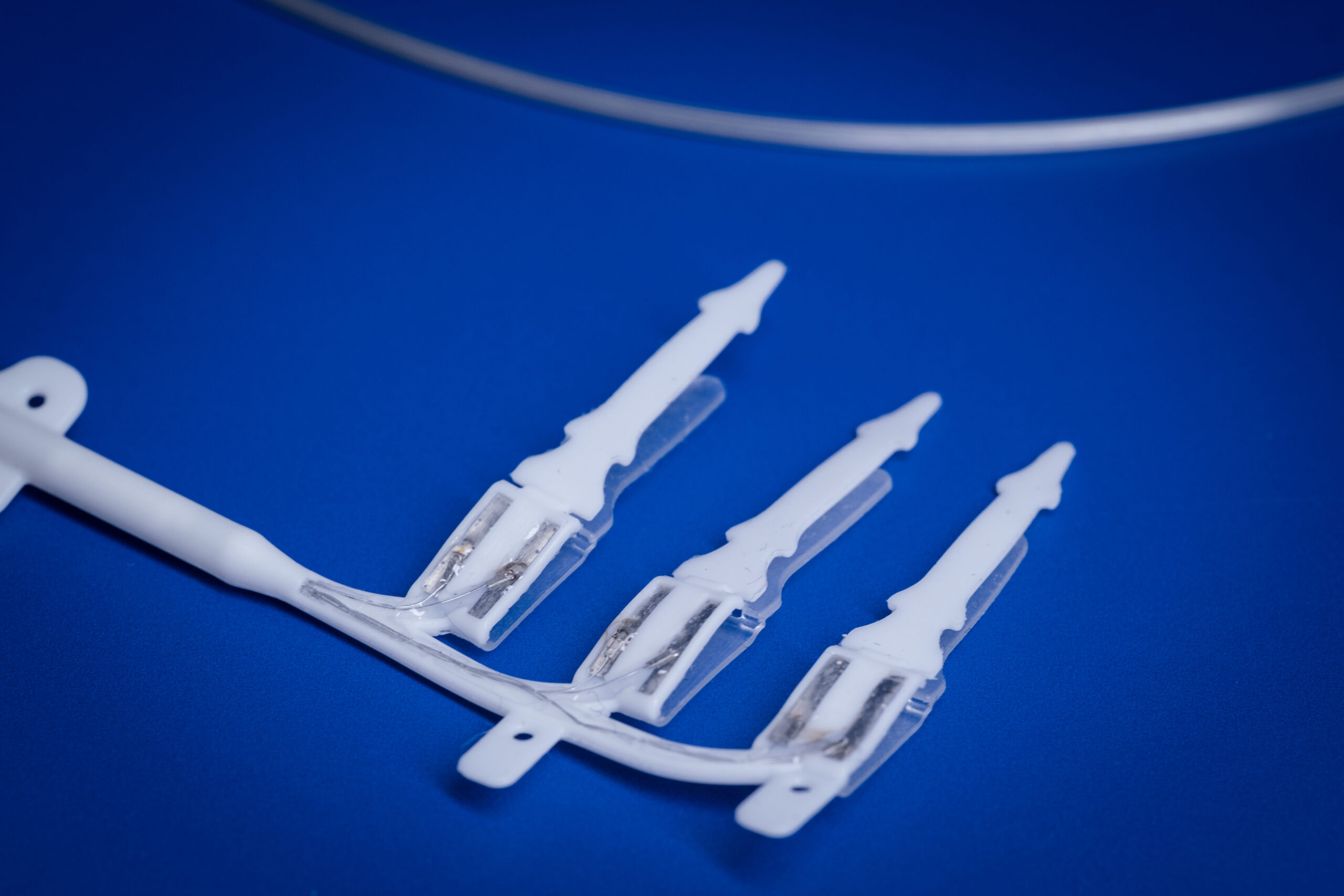
A multidisciplinary group of engineers and surgeons solved these problems by developing a human-machine interface that allows for the prosthesis to be comfortably attached to the user’s skeleton via osseointegration, while also enabling electrical connection with the nervous system via electrodes implanted in nerves and muscles.
“Karin was the first person with a below-elbow amputation to receive this new concept of a highly integrated bionic hand that can be used independently and reliably in daily life”, Professor Ortiz Catalán says.
“The fact that she has been able to use her prosthesis comfortably and effectively in daily activities for years is a promising testament to the potential life-changing capabilities of this novel technology for individuals facing limb loss.”
The challenges at this level of amputation are that the two bones (radius and ulna) should be aligned and loaded equally, and not much space is available for implanted and prosthetic components.
The research team nevertheless managed to develop a suitable neuromusculoskeletal implant that allows for connecting the user’s biological control system (the nervous system) with the electronic control system of the prosthesis.
An approach which Professor Ortiz Catalán says has benefits for those with phantom limb pain.
“Our integrated surgical and engineering approach also explains the reduction in pain, as Karin is now using somewhat the same neural resources to control the prosthesis as she did for her missing biological hand.”
Bionics Institute CEO Robert Klupacs says this research paves the way for people across the world with a below-elbow amputation to regain quality of life.
“This is an incredible step forward. This publication is evidence that combining sophisticated implanted electrodes, new microsurgical techniques and machine learning can provide a patient with a highly functioning bionic hand that they can control at will.
“We at the Bionics Institute are excited by what Professor Ortiz Catalán and his team of collaborators have achieved to date, and by their ongoing development of next generation bionic limb technology – particularly in light of its potential to assist with phantom limb pain relief,” he adds.
About the technology and osseointegration
A key feature of the new bionic technology is the skeletal attachment of the prosthesis via osseointegration; the process by which bone tissue embraces titanium creating a strong mechanical connection. Prof. Rickard Brånemark, research affiliate at MIT, associate professor at Gothenburg University, and CEO of Integrum, led the surgery and has worked with osseointegration for limb prosthesis since they were first used in humans.
“The biological integration of titanium implants into bone tissue creates opportunities to further advance amputee care. By combining osseointegration with reconstructive surgery, implanted electrodes, and AI, we can restore human function in an unprecedented way. The below elbow amputation level has particular challenges, and the level of functionality achieved marks an important milestone for the field of advanced extremity reconstructions as a whole,” Professor Rickard Brånemark explained.
The nerves and muscles in the residual limb were re-arranged to provide more source of motor control information to the prosthesis.
Dr Paolo Sassu (CBPR) conducted this part of the surgery that took place at the Sahlgrenska University Hospital in Sweden.
He said: “Depending on the clinical conditions, we can offer the best solution for our patients which sometimes is biological with a hand transplantation, and sometimes is bionic with neuromusculoskeletal prosthesis. We are continuously improving in both”.
The robotic hand, called Mia Hand, was developed by Prensilia and features unique motor and sensory components that allows the user to carry out 80% of the activities of daily living. “The acceptance of the prosthesis is critical for its successful use” says Dr. Francesco Clemente, Managing Director of Prensilia.
“Besides technical performance, Prensilia struggled to develop a hand that could be fully customiseable aesthetically. Mia Hand was born to be shown and not hidden. We wanted the users to be proud of what they are, rather than ashamed of what was lost.”
Funding
This work was one of the main outcomes of a project funded by the European Commission under Horizon 2020 called DeTOP (GA #687905). The research was also financed by the Promobilia Foundation, the IngaBritt and Arne Lundbergs Foundation, and the Swedish Research Council (Vetenskapsrådet).
“The DeTOP project, funded by the European Commission”, says coordinator Professor Christian Cipriani, from Scuola Sant’Anna, Pisa, “offered a great opportunity of collaboration which made possible the consolidation of state-of-art prosthetic and robotic technologies available in our institutions, that may have a terrific impact on people’s life”.
Collaborators
Paper authors include: Professor Max Ortiz Catalán, Head of Neural Prosthetic Research at the Bionics Institute in Australia, and Founding Director of the Center for Bionics and Pain Research in Sweden; Professor Rickard Brånemark, Research Affiliate at Massachusetts Institute of Technology, Associate Professor at Gothenburg University, and CEO of Integrum; Dr Paolo Sassu, Orthoplastic Consultant Surgeon, Istituto Ortopedico Rizzoli in Italy, and the Center for Bionics and Pain Research in Sweden; Dr Francesco Clemente, Managing Director of Prensilia.
Researchers are with the Center for Bionics and Pain Research (CBPR), a multidisciplinary collaboration between Sahlgrenska University Hospital, the Sahlgrenska Academy at the University of Gothenburg, and Chalmers University of Technology, all in Gothenburg, Sweden; the Bionics Institute in Melbourne, Australia; the Istituto Ortopedico Rizzoli, Bologna, Italy; the Scuola Superiore Sant’Anna, Pisa, Italy; TeamOlmed in Sweden; the University of Colorado, Aurora, USA; the Massachusetts Institute of Technology, Cambridge, USA; and the medical device companies Integrum AB in Sweden and Prensilia in Italy. The DeTOP project also included Lund University, the Swiss Center for Electronics and Microtechnology, INAIL Prosthetic Center, and Universitá Campus Bio-Medico.